This article will explore acamprosate for alcohol treatment. Acamprosate is a prescription medication that is used to help people manage post-acute alcohol withdrawal syndrome (PAWS).

The FDA approved acamprosate for alcohol dependence in 2004. This makes this medication one ofe the newest of the three FDA-approved medications for addiction (the others are disulfiram and naltrexone). It is sold under the brand name Campral Delayed Release Tablets.
Many people receiving this care report a reduction in post-acute withdrawal symptoms, including:
- Restlessness
- Insomnia
- Anxiety
- Cravings
We will now proceed to explore this medication and its treatment, including pharmacology, dosage information, research studies, and alternatives to this medication.
What is Acamprosate?
It may help to ameliorate post-acute withdrawal syndrome, with a notable impact for some people on anxiety and cravings. It does this by stabilizing brain chemicals involved in withdrawal.
Is Acamprosate Approved for Treating Alcoholism?
This is typically prescribed for 3-12 months following the cessation of acute withdrawal symptoms. This sets it apart from anticonvulsants (e.g., benzodiazepines) that are prescribed to prevent complications during withdrawal.
In Europe, it had been used with apparent success for decades before it was approved in the U.S.
In contrast to naltrexone, which blocks the pleasure that drinkers obtain – or disulfiram, which causes nausea when drinking – this medication relieves the intense sensation of stress that leads many alcoholics back to the bottle.
There is evidence that it works best for people who are committed to abstinence. However, people who “slip” while taking it for dependence are usually advised to continue taking the drug.
How Does Acamprosate Work?
While scientists still do not fully understand how it works, it is thought that acamprosate reduces glutamate activity in the brain.
Glutamate is a “stress” chemical that is suppressed by chronic drinking, and which rebounds to potentially dangerous levels when addicts attempt to quit cold turkey.
It may also modulate GABA activity, possibly indirectly through its action as a glutamate antagonist. GABA is the brain’s primary “calming” chemical.
In order to understand why this matters, it’s important to remember that alcohol mimics GABA (calming the brain) and suppresses glutamate (reducing stress). Withdrawal involves the opposite effect, which is also two-pronged: a lack of GABA and a surge of glutamate.
In the absence of drinking to calm down the brain, the alcoholic feels hyperactive, hypersensitive, and panicked. Many of the symptoms of withdrawal are caused by a lack of GABA and an excess of glutamate.
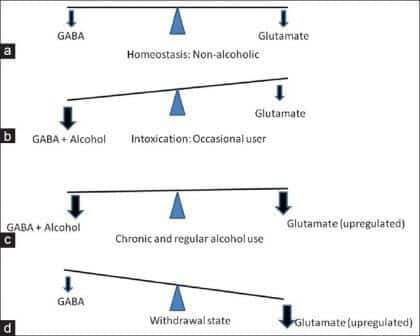
In the short term, benzodiazepines that stimulate GABA receptors are often used to resolve this chemical imbalance. However, benzodiazepines can lead to rapid tolerance and addiction. This medication is thought to be more useful for the long-term management of symptoms when this brain imbalance persists.
Dosage
The following dosage information may be useful if you are considering:
- A typical dose for dependence is 666 mg, three times per day.
- The brand name Campral comes in tablets of 333 mg, meaning that two tabs are often taken at once.
- The duration of the remedy is usually between three months and one year. (source)
- Only a doctor can determine your correct dosage depending on your situation.
- It may have interactions with other drugs, but there is no current data on these interactions.
- It does not cause an unpleasant reaction when consumed with alcohol.
- It is often taken on its own or in conjunction with benzodiazepines for withdrawal.
- Because everyone is biochemically different, some people do not respond well (or at all).
- Because It is not processed by the liver, it may be suitable for people with liver disease. However, because it is excreted by the kidneys, it should be avoided by people with severe kidney problems.
Before taking acamprosate for dependence, make sure to review the following:
Research Studies

A number of studies support the use of acamprosate:
- Of 272 alcoholic patients, half of whom received acamprosate for 48 weeks and half of whom received a placebo, the former group experienced a significantly higher abstinence rate. Higher abstinence for the former group continued during the following 48 weeks, during which no medications were given to either group. (source)
- This medication was shown to be well tolerated and very effective at increasing abstinence rates for alcoholic patients in a double-blind study, in which two dosages were used: 1,332 mg/day and 1,998 mg/day. Higher abstinence rates were noted with increased dosage. (source)
- In a study of alcoholics in real-world conditions, 540 individuals who received the medication were found to have a 33.6% abstinence rate compared to 21.6% for 274 individuals who received only psychosocial support. (source)
- A comprehensive meta-study of 17 trials consisting of 4,087 patients from 13 countries found that 36% of individuals receiving the medication and 23.4% of individuals receiving placebo remained abstinent at 6 months. (source)
- A study comparing this medication versus naltrexone for dependence concluded that this medication improves abstinence odds, with 77% of the acamprosate remaining abstinent versus 36% for naltrexone and 50% for placebo. (It should be noted that abstinence is not always the primary goal with naltrexone treatment.) (source)
- A critical review of studies found that this medication increases abstinence rates, reduces treatment costs, and produces superior results compared to group support alone. (source)
In addition to the above research, the following passage from the scientific literature is worth considering:
Discrepancies [in acamprosate’s effectiveness] may be mediated by genetic differences in the populations examined. For example, exciting emerging evidence suggests that alcohol effects are altered in mice carrying various mutations of the glutamatergic genes (see review by Gass and Olive 2008). If the effects of acamprosate are indeed mediated through this glutamatergic system, it would be worth examining these genetic markers as mediators of treatment response. Finally, patient-specific treatment matching also may enhance acamprosate’s efficacy. Evidence from a pooled analyses of seven European trials suggests that alcoholics with increased levels of anxiety, negative family history, and late age of onset of alcoholism, as well as those who are women, may benefit from this medication (Verheul et al. 2005).
Alternatives
Not everyone can obtain acamprosate since it must be prescribed by a doctor.
Besides benzodiazepines, which are the most commonly prescribed drugs for short-term alcohol detox, there are a few other alternatives.
You can read some other articles on prescription medications for withdrawal and cravings here:
Further Considerations – Nutritional Repair

After getting through acute withdrawal, it’s important to determine what lifestyle changes will reduce cravings and repair the body-brain system.
Nutrition is one of the most neglected pillars of recovery. After removing toxic ethanol from your life, you can maximize your sense of well-being by optimizing what you put into your body. This includes eating well and taking supplements to repair nutritional deficiencies.
Check Fit Recovery’s list of supplements that work best for supporting the brain-body system through recovery.
Conclusion
People with substance abuse disorders deserve to know about all of their options for changing their lives for the better.
There is no one-size-fits-all approach to detox and recovery. Most people who quit are not informed about nutrient repair, pharmacological support, or holistic strategies for improving their quality of life.
If you have any questions about acamprosate for alcohol treatment, please leave them in the comment box below.
___________________________________

Dr. Ken Starr is board-certified in both Addiction Medicine and Emergency Medicine, and diplomate of the American Board of Addiction Medicine. In addition to his work as the Addiction Medicine Director for Fit Recovery, he operates Ken Starr MD Wellness Group in Arroyo Grande, CA. His clinic offers advanced drug and alcohol detox methods, long-term recovery facilitation, and IV nutritional programs including NAD+ therapy.

Author
-
 View all posts
View all postsDr. Ken Starr is board certified in both Addiction Medicine and Emergency Medicine, and diplomate of the American Board of Addiction Medicine. In addition to his work as the Addiction Medicine Director for Fit Recovery, he operates Ken Starr MD Wellness Group in Arroyo Grande, CA. His clinic offers advanced drug and alcohol detox methods, long term recovery facilitation, and IV nutritional programs including NAD+ therapy.







Hi Chris. Lot’s of great info here. Just a quick question. I tend not to drink for a month or so then drink heavily morning til night for about 10-14 days. I’m fine for the first few days, but after that I’m drinking just to avoid the hangover which is 95% mental (brain fog, boredom, anxiety). I don’t get any cravings whatsoever during the sober periods, but once i start the bar is like a strong magnet pulling me in as soon as i wake and it usually takes me a few days to be able to sleep after I… Read more »
Hi AD, great question and I can relate to your situation. If you were to be prescribed Campral, a doctor would have to determine the correct dosage because many factors are involved (bodyweight, tolerance, etc.). The cycle that you are describing occurred to me when I was younger, and I wish someone had told me that eventually the sober periods would imperceptibly shrink to a few weeks, then a week, then a few days, then a few hours. So I think it’s smart that you want to nip this cycle in the bud. If I were you, I would begin… Read more »
Very good article. I have a Masters in Psychology and have suffered for many years with alcohol abuse. I finally went into a day rehab centre and was told there by many patients that Acamprosate had worked on them, so just started taking it myself. It’s unbelievable that there is so little information out there on it and like you, none of the numerous doctors I saw about my alcohol problem told me this even existed or was an option. There should be more awareness of it and how it differs drastically from Naltrexone and Antabuse (Disulfiram).
Thanks Gaby, it’s very frustrating that the treatment options for alcoholism are rarely presented in their entirety.
I’m glad you enjoyed the article and nice work on being proactive yourself! Best of luck to you, and stay posted for more.
Excellent info. I will read it a few times.
I am 62 and I began drinking at 16. My problem is more ‘binge’, 2-3 times a month. I’m ok if I stay away but, in a bar, if I drink 6 beers, I must have 6 more. Would Campral help here? I’m seeing a counsellor but I cannot develop adequate self-discipline. Thank you.
John Duffy
Ireland
Thanks John – Campral may help if you suffer from anxiety or depression that causes you to binge drink. However, it is usually prescribed for people who have had a hard time withdrawing from alcohol. It sounds like your binge drinking might be helped by The Sinclair Method, which involves taking naltrexone prior to drinking. Over time, naltrexone helps to extinguish the desire to drink excessively. A growing number of doctors are open to prescribing naltrexone for alcohol problems – although it can still be hard to find one, depending on where you live. I can assure you that you’ll… Read more »