In this article, we will review the effects, interactions, and addiction potential for both alcohol and benzodiazepines. These drugs have some similarities in how they affect our systems, but also some pronounced differences.

Both of these reduce brain activity by stimulating GABA receptors. Generally, alcohol is a more complicated drug than benzodiazepines because it affects more neurotransmitters.
We will now proceed to overview both. After that, we will cover the effects of combining these drugs, the use of this medication for withdrawal, and some alternatives that can be used to achieve similar effects or address a deficiency in GABA production.
Overview
Overview Of Alcohol
Alcohol is a central nervous system depressant that is very similar in structure to GABA, which is the brain’s primary calming neurotransmitter. It also activates the brain’s mu and kappa opioid receptors. (source) In turn, alcohol releases dopamine and raises levels of serotonin. Its effects on the brain are far-reaching and complex.
The most common side effects of alcohol include:
- Relaxation
- Euphoria
- Disorientation
- Sedation
- Hangovers
- Dependence
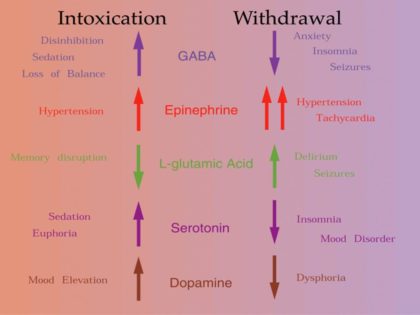
Because of biochemical individuality, different people respond to drinking in different ways. I became addicted very quickly and at a relatively young age. For people who become addicted, the effects of prolonged drinking can become very severe:
- High blood pressure
- Pancreas inflammation
- Liver cirrhosis
- Brain damage
- Damaged immune system
- Increased stroke risk
- Increased cancer risk
The liver breaks down alcohol into water, acetic acid, and acetaldehyde. This last compound is a poison that is responsible for hangovers and free radical damage to bodily cells, increasing inflammation and the risk of cancer.
The addictive potential seems to strongly correlate with individual biochemical makeup, which is determined by genes – and which are, in turn, activated by environmental factors such as lifestyle. About 88,000 Americans die each year of alcohol-related causes. (source)
Overview Of Benzodiazepines
Benzodiazepines are prescription drugs that are used to reduce anxiety, prevent convulsions, and help with sleep. Because they vary in terms of strength and length of effects, doctors choose between them depending on the patient’s symptoms. Common benzodiazepine brands include Xanax, Valium, Librium, Ativan, and Klonopin.
They are effective for alleviating or preventing the following symptoms:
- Anxiety
- Insomnia
- Restlessness
- Panic attacks
- Tremors
- Muscle spasms
- High blood pressure
They work by activating GABA receptors in the brain. GABA is an inhibitory neurotransmitter associated with feelings of calm. This neurotransmitter essentially dampens brain activity, helping to regulate levels of glutamate, which increases the amount of electrical activity in the brain. Normalized brain chemistry requires stable levels of both GABA and glutamate.
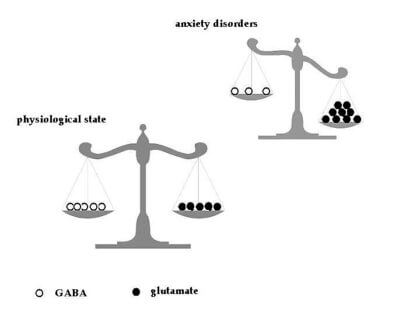
They are most commonly prescribed for anxiety disorders. Most people take these drugs to help deal with situational stressors or for short time periods. However, in recent years, more people have begun taking them for extended durations (classified as over 4 months).
The use of them is strongly correlated with age. About 5% of young adults have prescriptions for these drugs, with the number rising to 10% for people 65 and older. About a third of these older adults have prescriptions that are indicated for long-term use. (source)
Some pronounced side effects include:
- Drowsiness
- Confusion
- Dizziness
- Cognitive impairment
- Blurred vision
- Weakness
- Difficulty breathing
- Dependence
All benzodiazepines are known to cause dependence when used for extended periods of time. Therefore, doses should never be stopped abruptly. Benzodiazepine withdrawal symptoms are very similar to the symptoms of withdrawal, because both of these drugs cause profound changes in GABA/glutamate levels over time.
Rates of benzodiazepine addiction have risen in recent years. Addiction to these drugs is less punishing on the body than addiction, but it can heavily skew neurotransmission and lead to confusion, depression, aggression, and increased risk of suicide. Over 90% of people who enroll in treatment centers for benzodiazepine addiction also suffer from either opiate addiction or addiction.
Combination & Interactions
Because alcohol and benzodiazepines act on the same brain receptors, they are said to have cross-tolerance. Combining them potentiates the effects of both of these drugs. In particular, people who take this medication along with alcohol are more likely to experience:
- Blackouts
- Unconsciousness
- Coma
- Organ failure
- Death
As a general rule, it’s best to avoid ever combining these substances. Of course, this doesn’t mean that most people who are dependent on either of these substances observe this rule. It’s good to know that habitually combining these drugs (and alcohol is certainly a drug) can increase their respective effects, risks, and potential for addiction.
Use of Benzodiazepines For Withdrawal

Intoxication causes a spike in GABA and withdrawal involves a plunge in GABA. Many withdrawal symptoms (including panic and even seizures) are caused by insufficient levels of GABA in the brain. Therefore, benzodiazepines are often extremely effective for relieving withdrawal.
Using them for withdrawal can provide temporary peace of mind and prevent severe symptoms from manifesting. Because of its effectiveness for withdrawal symptoms, hospitals often prescribe these drugs to addicts and then gradually reduce the dose to taper them off.
You can read more about the use of this medication for withdrawal in these articles:
Alternatives to Alcohol and Benzodiazepines

Both help people reduce short-term stress by stimulating GABA receptors. However, for people with addictions to these substances, the long-term effects (including addiction) tend to cancel out the short-term benefits.
Want to increase your levels of GABA naturally? Here are a few ways you can achieve this naturally:
- Swedish massage
- Yoga classes
- Exercise daily
- Get better sleep
- Clean up your diet
- Supplement with L-Glutamine
- Try natural kava
Conclusion
We hope you’ve taken useful information from this article. If you struggle with dependence, you will benefit from immersing yourself in Fit Recovery.
Check Fit Recovery’s list of supplements that work best for supporting the brain-body system through recovery.
If you have any questions, please leave them in the comment box below.
___________________________________

Dr. Ken Starr is board certified in both Addiction Medicine and Emergency Medicine, and diplomate of the American Board of Addiction Medicine. In addition to his work as the Addiction Medicine Director for Fit Recovery, he operates Ken Starr MD Wellness Group in Arroyo Grande, CA. His clinic offers advanced drug and alcohol detox methods, long term recovery facilitation, and IV nutritional programs including NAD+ therapy.

Author
-
 View all posts
View all postsDr. Ken Starr is board certified in both Addiction Medicine and Emergency Medicine, and diplomate of the American Board of Addiction Medicine. In addition to his work as the Addiction Medicine Director for Fit Recovery, he operates Ken Starr MD Wellness Group in Arroyo Grande, CA. His clinic offers advanced drug and alcohol detox methods, long term recovery facilitation, and IV nutritional programs including NAD+ therapy.





